Bloating: Causes, Quick Fixes, and When to See a Doctor
Bloating makes your belly feel tight, swollen, or uncomfortable. It happens to almost everyone. Some cases clear in a few hours. Others stick around and affect daily life. Here’s a practical, easy guide to find likely reasons and simple steps you can try today.
Common causes include gas from swallowed air or fermentation, constipation, meals high in FODMAPs (like beans, onions, apples), and food intolerances such as lactose. Certain medications and supplements can also cause bloating. For example, some painkillers, antibiotics, and supplements that change gut bacteria may lead to trapped gas or slowed digestion.
Fluid retention is a different kind of swelling. If your belly feels puffy and your legs or hands also swell, it might be fluid buildup. That can be related to heart, kidney, or liver issues. Our articles on Lasix alternatives and edema explain options if a diuretic is being considered.
Quick fixes to try at home
Move more. A 10–20 minute walk after a meal often helps move gas and speed digestion. Drink warm water or herbal tea like peppermint — it can relax the gut and ease bloating. Cut down on carbonated drinks and straws; they add swallowed air. Eat slowly and chew well. Smaller meals spaced out through the day often feel better than two giant ones.
Try an over-the-counter remedy for gas, like simethicone, for short-term relief. If constipation is the issue, gentle fiber increases and an osmotic laxative for a short period may help. Probiotics help some people, but pick one with strains shown for bloating and give it a month to see if it helps.
When to see a doctor
Talk to a doctor if bloating is severe, happens suddenly, or follows weight loss, ongoing vomiting, blood in stool, or trouble swallowing. Also get checked if you have persistent abdominal pain or fever. These signs could mean an infection, bowel blockage, or other serious issues. If your doctor thinks acid reflux or GERD is causing symptoms, they may discuss acid-suppressing options — see our guide on esomeprazole alternatives for different approaches.
Keep a simple food and symptom diary for two weeks. Note what you eat, how much, and when bloating hits. That helps you and your doctor spot patterns, like lactose intolerance or sensitivity to high-FODMAP foods. If medications are the likely cause, don’t stop them on your own. Ask your provider about safer alternatives or dose changes.
Try a 2–4 week low-FODMAP trial if you suspect food triggers. Cut out sorbitol and xylitol (found in sugar-free gum) because they often cause gas. If bloating follows antibiotics, ask about probiotic timing. For ongoing or worsening symptoms your doctor may order tests like breath testing for SIBO or imaging to rule out other causes. Use food diaries.
Bloating is common and usually manageable with small lifestyle changes. But persistent or severe cases deserve a medical check. Use simple tests, a clear history, and focused treatments to get back to feeling normal.
 9 May 2023
9 May 2023
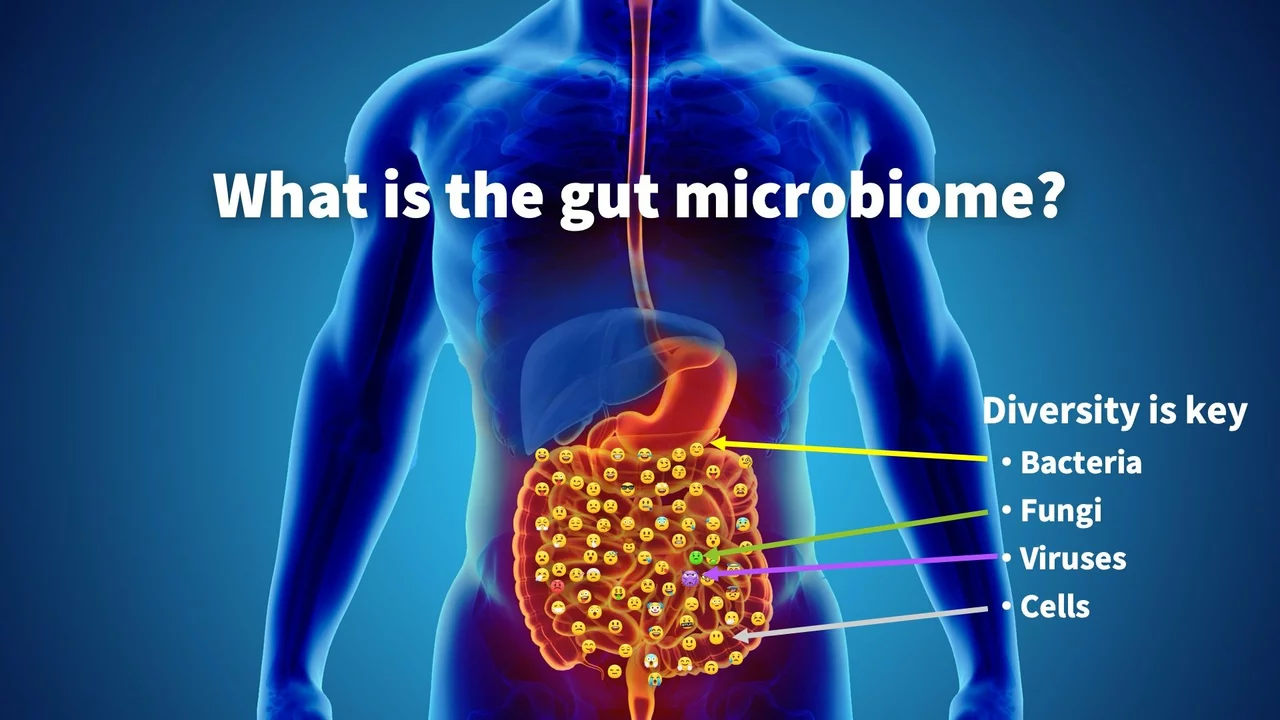
Bloating after a meal: the importance of a balanced gut microbiome
I recently explored the topic of bloating after a meal, and discovered that a balanced gut microbiome plays a crucial role in preventing this uncomfortable sensation. It turns out that the right balance of good and bad bacteria in our gut helps break down food efficiently and reduces gas production. Not only does a healthy gut microbiome aid in digestion, but it also supports our overall well-being. Incorporating probiotics and prebiotics in our diet can help maintain this delicate balance. So, the next time you feel bloated after a meal, remember to consider the importance of a balanced gut microbiome for better digestion and health.
Latest Posts
-

Smoking and Heart Disease: Proven Cessation Strategies That Save Lives
-

Digestive Enzymes: When Supplements May Help GI Symptoms
-
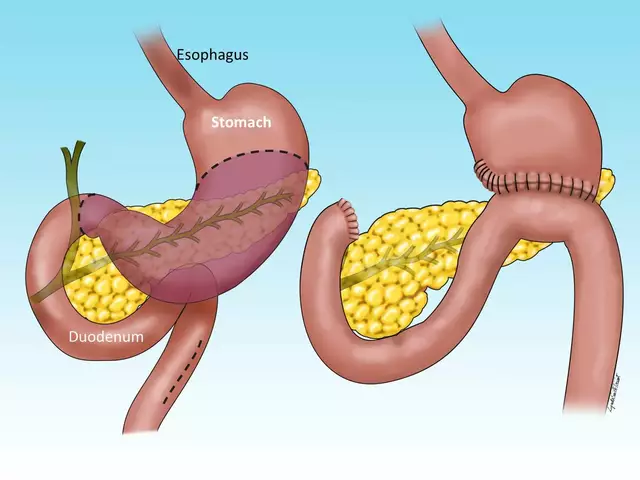
The Importance of Regular Checkups for Atrophic Gastroenteritis Patients
-

Authorized Generic Pricing: Why They Cost Less Than Brand Name Drugs
-

Boost Your Overall Health with the Power of Fructo-Oligosaccharides Dietary Supplement

9