Intravenous therapy: what you need to know
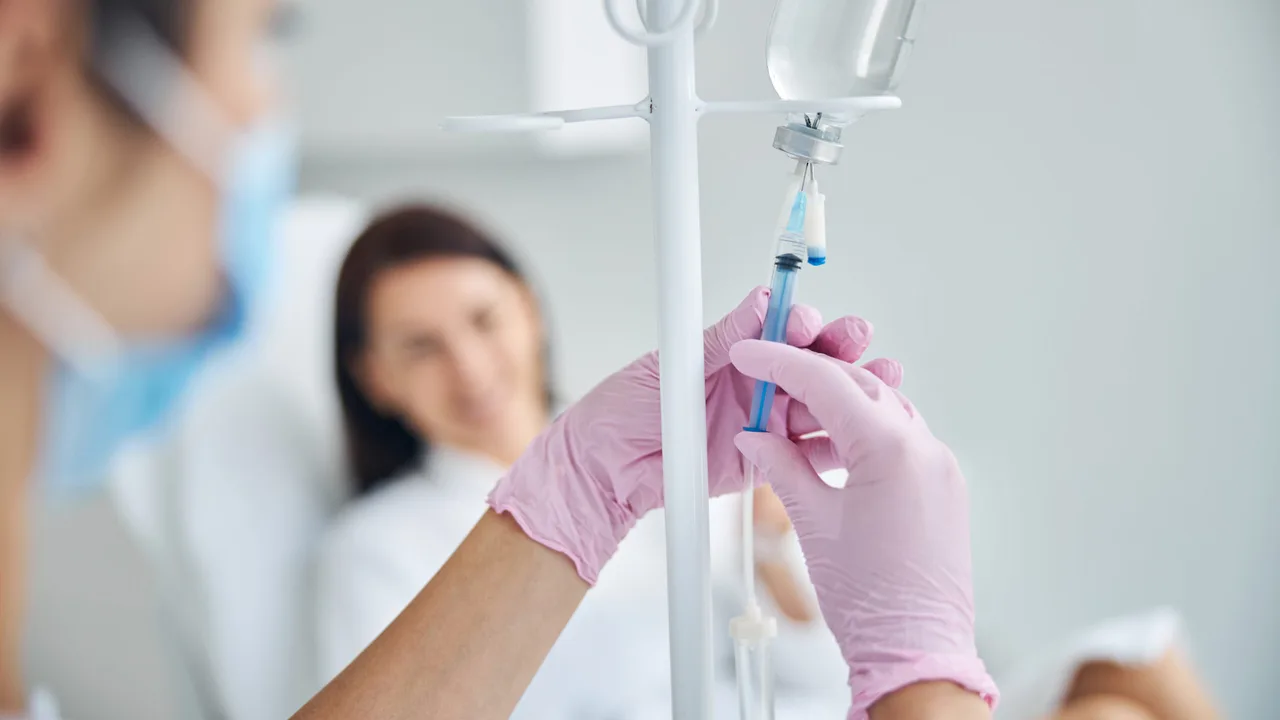
Intravenous (IV) therapy delivers fluids, medications, or nutrients directly into a vein. It works fast and is used in hospitals, clinics, and some home-care settings. IV therapy can correct dehydration, give antibiotics, control pain, replace electrolytes, and provide chemotherapy or nutrition when eating is not possible.
When IV therapy is used
Doctors choose IV therapy when oral treatment is too slow, not tolerated, or not possible. Common reasons include severe infections, major surgery, dehydration from vomiting or diarrhea, cancer treatments, and emergencies like shock. IV lines also make it easier to give repeated doses without repeated needle sticks.
Types of IV access
There are several kinds of IV access. Peripheral IVs are short catheters placed in hand or arm veins for short-term use. Midline catheters are longer and sit in larger arm veins for a few weeks. Central lines and peripherally inserted central catheters (PICCs) reach large veins near the heart and suit long-term therapies. Each type has pros and cons depending on treatment length and drug properties.
Starting an IV takes skill. A trained nurse or doctor will clean the skin, choose a vein, and insert a catheter. You may feel a quick sting. Once the catheter is secure, tubing and a bag or syringe deliver the fluid or drug at a controlled rate. Pumps may be used to keep flow steady.
Know the risks so you can watch for problems. Common issues include local pain, bruising, and infection at the insertion site. More serious risks are phlebitis (vein inflammation), bloodstream infection, air embolism, and fluid overload. Risk rises with longer use and with central lines. Report fever, increasing pain, swelling, redness, leakage, or shortness of breath right away.
There are simple steps you and staff can take to reduce risk. Clean hands and sterile technique matter. Keep the site dry and check dressings daily. Avoid tugging on tubing. Follow instructions about showering and activity. If you receive IV care at home, make sure staff are trained and you know how to get emergency help.
IV therapy requires monitoring. Nurses check the infusion rate, site condition, and patient symptoms. Labs may test electrolytes, kidney function, and drug levels to adjust treatment. Communication helps: tell your team about allergies, previous IV problems, or if you feel unusual symptoms during infusion.
For many treatments, alternatives exist. Oral medicines, injections into muscle, or subcutaneous infusions can work instead of IV in some cases. Ask your clinician whether IV is necessary and what options fit your situation. Understanding the reason and plan makes the process less stressful.
If you have questions about a specific IV drug or line type, bring them up before treatment. Knowing why a drug is given, how long the IV will stay in, and what side effects to expect helps you stay safe and comfortable. Good communication and simple precautions make IV therapy effective and much safer. Keep notes of dates and any problems so follow up care stays clear and documented.
 8 November 2023
8 November 2023
The Role of Intravenous (IV) Therapy in Leukemia Treatment
Hi there, I'm getting into a pretty heavy topic today - the role of intravenous (IV) therapy in leukemia treatment. It's a critical component that makes a huge difference in patient recovery. Through this post, I'll shed some light on how IV therapy works, its importance, and why it's a preferred method for cancer care. Join me as we delve deeper into understanding this approach in our fight against leukemia.
Latest Posts
-

The Crucial Role of Fluconazole in Managing HIV/AIDS
-

The role of adapalene in treating acne on darker skin tones
-

CYP450 Enzyme Interactions: How Medications Compete for Metabolism
-

Rifampin and Hormonal Contraceptives: Breakthrough Ovulation Risk
-

Stereospermum Plant Guide: Uses, Health Benefits, and Growing Tips

13